Current Trends In The Treatment Of Erectile Dysfunction

Introduction:
Remarkable progress has been made in the field of Erectile Dysfunction (ED) management, encompassing all areas of epidemiology, basic scientific research, clinical investigation, and health services research during the last three decades. Majority of cases of ED are due to vascular causes although it can be associated with other pathology. Currently, after excluding other possible causes and contraindication, the first line of treatment is medications like phosphodiesterase type 5 (PDE5) inhibitors. However, they are successful only in 50% to 70% of cases. As the dysfunction can be due to more than one cause, combination of different modalities of treatment can be required in selected cases.
Various Modalities of Treatment
Treatment must be tailored according to the underlying cause. Therefore, the clinician must have a good knowledge of pathophysiology of ED. And to be successful, the patient and partner or wife must be compliant and co-operative.
The first step is to correct reversible causes that can provoke failure of erectile function.
These include alteration of lifestyle like stopping of smoking and reduction of alcohol intake. It is also important to reduce stress and exhaustion.
In some cases, change of medications that can impair erectile function is essential.
1. Psychosexual therapy
This is to understand and address underlying psychological issues and provides information and treatment in the form of sex education, psycho- sexual counseling, instruction on improving partner communication skills, cognitive therapy, and behavioural therapy (programmed relearning of couple’s sexual relationship). Pharmacotherapy may be a useful adjuvant.
2. Drug therapy
(a) Phosphodiesterase type-5 (PDE5) inhibitors:
first-line therapies which include sildenafil (Viagra, Caverta) , tadalafil (Cialis, Duron) , vardenafil (Levitra) . PDE5 inhibitors enhance cavernosal smooth muscle relaxation and erection by blocking the breakdown of cGMP by phosphodiesterase. Sexual stimulus is still required to initiate events. Success is reported in up to 70% if the cases are properly selected. Early use of PDE5 inhibitors following radical prostatectomy can help optimize the return of spontaneous erections (penile rehabilitation).
Contraindications include patients taking nitrates, recent myocardial infarction, recent stroke, hypotension, unstable angina, non-arteritic anterior ischaemic optic nerve neuropathy (NAION). Cautions: intermediate and high risk cardiovascular disease requires cardiac review prior to treatment. Patients should be warned that overdose can lead to to priapism.
A comparison of PDE5 inhibitors:
(a) Sildenafil – Action starts at 30–60 min, lasts Up to 4–5h
SE: Headache, dizziness, GI upset, flushing, nasal congestion, blurred vision
(b)Vardenafil – action starts at 25–60 min, lasts Up to 4–5h, SE As above
(c)Tadalafil – action starts at 30 min, lasts Up to 36h,SE As above
(b) Dopamine receptor agonist:
Apomorphine (Uprima) taken sublingually, acts centrally on dopaminergic receptors in the paraventricular nucleus of the hypothalamus to enhance and coordinate the effect of sexual stimuli. Side effects include nausea, headache and dizziness. It is not commonly used.
When treatment with PDE5 inhibitors is contraindicated or failed totally or does not provide a satisfactory outcome, there are other treatment options: some are non- invasive, others are minimally invasive and some others are invasive.
Treatment can be given as a single modality or combined depending on the underlying cause or causes of the patient.
- Intraurethral therapy: second-line therapy when oral therapies have been ineffective. A synthetic prostaglandin E1 (PGE1) pellet (alprostadil) is placed into the urethra via a specialized applicator (Medicated Urethral System for Erection (MUSE) TM device). Once inserted, the penis is gently rolled to encourage the pellet to dissolve into the urethral mucosa from where it enters the corpora. PGE1 acts to increase cAMP within the corporal smooth muscle, resulting in muscle relaxation. Side effects: penile and urethral pain, priapism and local reactions. Fig :1
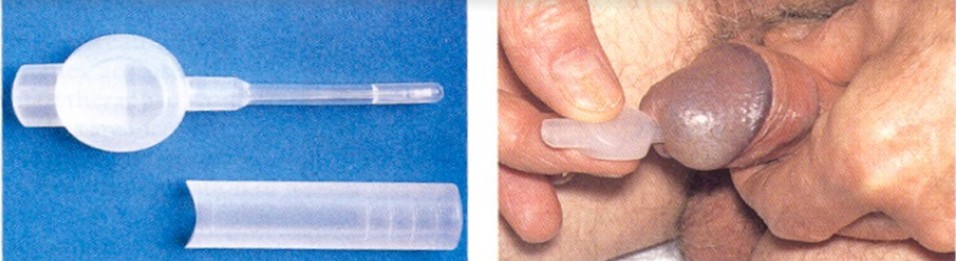
Fig 1.Intraurethral PGE1
2. Intracavernosal vasoactive substance injection therapy
- Alprostadil (CaverjetTM)
- Papaverine (PDE inhibitor). Usually given in combination with eitherphentolamine (A-adrenoceptor antagonist) or PGE1 in patients who have failed oral or single-agent injectable therapies.Training of technique and first dose is given by urologist. Needle is inserted at right angles into the corpus cavernosum on the lateral aspects of mid-penile shaft. Discontinuation rates from penile injection techniques are high. Contraindications: sickle cell disease or high-risk candidate for priapism. Adverse effects: pain, priapism, haematoma.
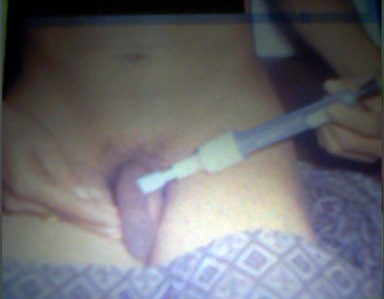
Fig. 2aIntracavernosal vasoactive substance injection
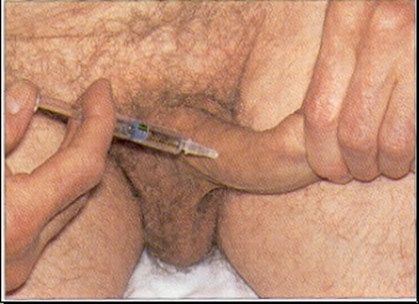
Fig. 2bIntracavernosal vasoactive substance injection
3.Vacuum Erection Device(VED)
It is used when pharmacotherapies have failed. It contains three components: a vacuum chamber, pump, and constriction band. The penis is placed in the chamber and the vacuum created by the pump increases blood flow to the corpora cavernosa to induce an erection. The constriction band is placed onto the base of the penis to retain blood in the corpora and maintain rigidity. Relative contraindications include anticoagulation therapy. Side effects: penile coldness, bruising.
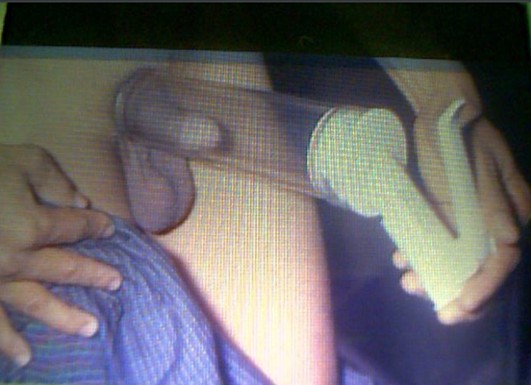
Fig 3 : Vacuum Erection Device
4.Microvascular arterial bypass and venous ligation surgery
These procedures are performed in specialist centres where there is a clear-cut diagnosis of a vascular disorder. Acts to increase arterial inflow and decrease venous outflow. Rarely used now as it is uncommon for success rates to exceed 50%.
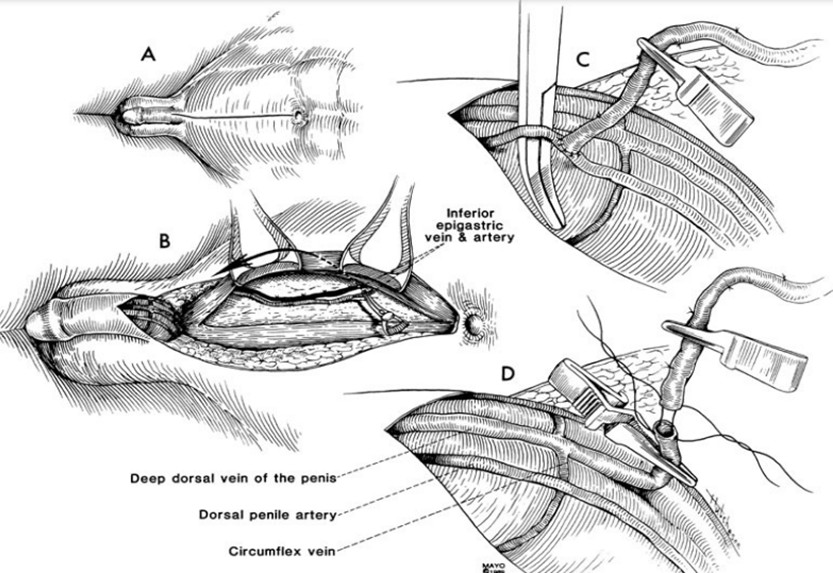
Fig :4 Arterial surgery – Anastomosis between Inferior Epigastric Artery and Dorsal Vein of Penis
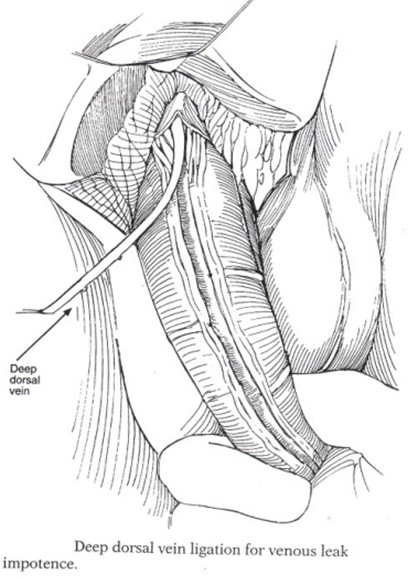
Fig: 5 Venous surgery (Dorsal Vein of Penis Ligation) for defective veno-occlusive mechanism
5.Penile prosthesis
Semi-rigid, malleable, and inflatable penile prostheses are available when other therapies have failed or are unsuitable. Also indicated for Peyronie’s disease, trauma, and penile fibrosis (i.e. secondary to priapism). The device is surgically implanted into the corpora to provide penile rigidity and generally has high satisfaction rates, up to 90% .
Side effects: infection, erosion, mechanical failure and penile shortening . Sometimes, glans may not fully engorge.
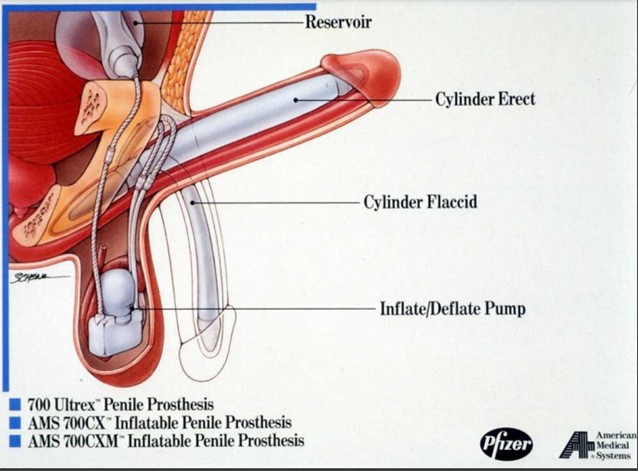
Fig 6. Penile Prosthesis
6.Low intensity Focus Ultrasound
This procedure has come into clinical practice since the last 7 years. Low intensity focus ultrasound causes new vessel formation in cavernosal arteries. This is a non-invasive treatment and is repeatable.The success rate of this treatment modality is 54% to 65%.
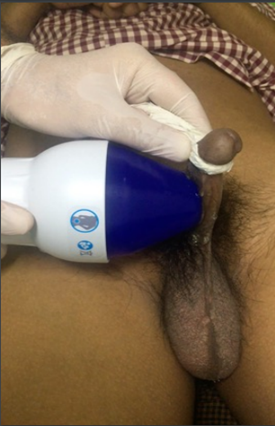
Fig 7: Low intensity Focus Ultrasound
7.Testosterone replacement therapy
It is indicated for hypogonadism and is available in oral, buccal, intramuscular, pellet, transdermal patch, and gel forms. Most guidelines recommend PSA, Hb, and LFT checks before and after starting treatment. It can improve the results of PDE5 inhibitors in hypogonadal men.
Future Directions
Future directions will assuredly continue with particular interest directed to new therapeutics. In the near future, pharmacotherapies will likely remain center stage, further driven by research discoveries in the molecular and cellular mechanisms responsible for the erectile response. Technologic advances in the way of interventional devices have rapidly gained interest. Alternatives such as implanting zotarolimus-eluting peripheral stents in atherosclerotic lesions of
the internal pudendal arteries and low-intensity extracorporeal shockwave therapy applied to the penis are currently under study, supporting the idea that these andother such interventions may achieve the goal of restoring erectile function or improving it effectively for the long term. Futuristic approaches such as gene therapy, stem-cell therapy, and tissue engineering have been mainly advanced at the preclinical stage of development with the same long-term purpose, although their eventual roles remain eagerly anticipated.
Suggested readings:
Bhasin S, Cunningham GR, Hayes FJ, et al. Testosterone therapy in men with androgen deficiency syndromes: an Endocrine Society clinical practice
guideline. J ClinEndocrinolMetab 2010;95:2536–59.
Gon, L.M., de Campos, C.C.C., Voris, B.R.I. et al. A systematic review of penile prosthesis infection and meta-analysis of diabetes mellitus role. BMC Urol 21, 35 (2021).
Khera M, Goldstein I. Erectile dysfunction. ClinEvid (Online) 2011;Jun 29:1803.
Lewis RW, Fugl-Meyer KS, Corona G, et al. Definitions/epidemiology/risk factors for sexual dysfunction. J Sex Med 2010;7:1598–607.
Montague DK, Jarow JP, Broderick GA, et al. Chapter 1: the management of
erectile dysfunction: an AUA update. J Urol 2005;174:230–9.
Montorsi F, Adaikan G, Becher E, et al. Summary of the recommendations on sexual dysfunctions in men. J Sex Med 2010;7:3572–88.
Porst H, Burnett A, Brock G, et al. SOP conservative (medical and mechanical)
treatment of erectile dysfunction. J Sex Med 2013;10:130–71.
Author Information
Toe Lwin
FRCS, FACS, Dr.Med.Sc
Honorary Professor, Department of Urology, University of Medicine1, Yangon





