Understanding Dehydration


Introduction
Cells are made up of about 80-85% of water, and are surrounded by water. Optimum functioning of cells is achieved by a stable internal environment (internal milieu) maintained by various homeostatic mechanisms. Just the correct amount of glucose, colloids, crystalloids, electrolytes, adequate oxygen, and water, correct range of pH are essential. Dehydration occurs when more water and fluids leave the body than enter it. Often because water intake is not the most pressing topic for the average clinical visit, it is often overlooked regarding patient care, It is not impossible for in-patients in specialist care settings to be dehydrated unnoticed by the various specialists focusing on their specific areas of expertise. It can happen and has happened, though infrequently. Water balance does not belong to any particular specialty; yet it encroaches every domain of patient care.
The population at large may also be dehydrated, unnoticed by anybody. It has been reported to occur in 17% to 28% of older adults in the United States.1It could be higher in tropical climates, especially in the elderly because the thirst mechanism is less sensitive as we age. Young children and unconscious patients are also at greater risk of dehydration although healthy young adults with easy access to water are rarely dehydrated.
An inadequately hydrated patient is put at a disadvantage. It is important that healthcare providers are cognizant of the aetiology, pathogenesis and management of dehydration in order to provide the best care possible.
The body fluids compartments
The total body water (TBW) 2 is about 60 per cent of body weight in normal adult males of normal weight and 55% in adult women.. Obese individuals have less TBW and infants have more (75-80%), making them more vulnerable to the effects of fluid loss. TBW exists in three body fluids compartments: intracellular fluid compartment (ICF), intercellular / interstitial fluid compartment (ISF) and intravascular fluid compartment (IVF) which is the plasma. The ICF is 2/3 of the TBW and ECF (ISF +IVF) one-third. Of the ECF, ISF makes up three-quarters of ECF and IVF a mere quarter. An adult man weighing 70 kg has a body volume of 70 litres. His TBW is 60% of 70 litres or 42 litres. His ICF would be 28 litres, ISF 10.5 and IVF 3.5 litres.
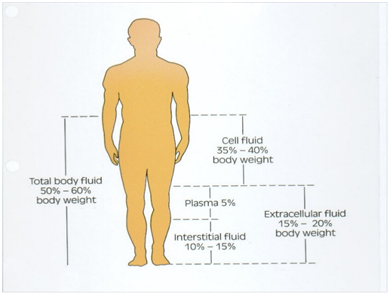
Fig.1-The body fluids compartments
The plasma osmolality is 280 + 5 mOsm/Kg, easily calculated as Posm =2 [Na(+)] +glucose(mg/dL)/18+BUN (mg/dL)//2.83 The IVF. being in communication with the gut, kidneys, skin and lungs, is the most variable, receiving water from and losing water to the gut; and losing water through the remaining three routes.
The body fluids are separated by a semi-permeable membrane which prevents proteins from leaving the cells or the IVF. The water, colloids and crystalloids are kept in their compartments maintained by the Donnan equilibrium. Fluid shifts between compartments, pulled by osmosis and pushed by hydrostatic pressure. The ISF is formed from the plasma, governed by the Starling forces (pull by osmotically active substances and pushed by hydrostatic pressure). About 24 litres are formed per day. Oedema is a condition of increased formation of ISF.
Whenever the IVF volume or osmolality is disturbed, the derangement is shared between the IVF and ISF, and thence with the ICF if equilibrium has not been reached. For example, drinking a litre of water would increase the IVF volume and reduce the osmolality. The higher osmotic pressure in the ISF pulls water from IVF. The added volume and reduction in osmolality are shared between the IVF and ISF. If the osmolality is still lower than normal, water moves by osmosis into the cells. On the other hand, loss of water from the IVF causes contraction of IVF and raised osmolality. Water is pulled from ISF, and thence from the ICF.
Water balance
Water is gained only from the gut (drinking and reabsorption of gastrointestinal secretions); the water produced by metabolism is negligible. It is lost through the lungs, skin, kidneys and gut. The gut secretions add up to around 9.2 litres but the faeces contain only around 0.2 litres normally. The amount lost is increased with diarrhoea, vomiting and fistulae. Loss through the lungs is around 0.3 litres per day but is increased with hyperventilation or in fever. Loss through the skin in the absence of sweating (“insensible perspiration”) is about 0.6 litres but can be increased with sweating (estimated to be 3-4 litres per day in the hot season). Thus, the minimal amount lost per day is around 1.1 litres
(0.3 from the lungs, 0.6 from the skin and 0.2 I in faeces) .The minimum fluid intake should therefore be 1.1 litres + urine volume. Extra losses in diarrhoea, vomiting, hyperventilation, kidney disease, endocrine disorders need to be taken into consideration.
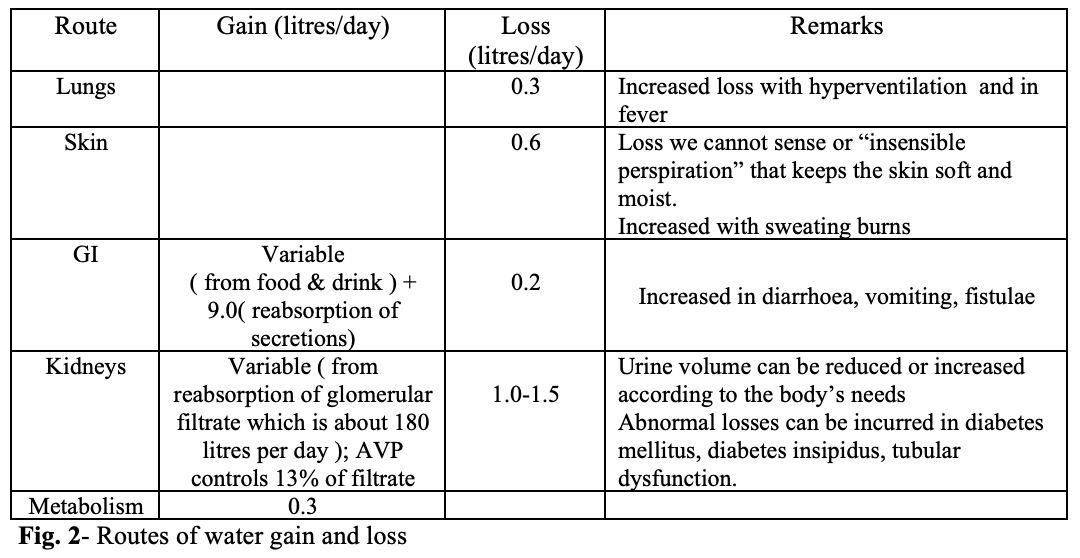
It should be noted that of the four routes of communication with the outside world, the kidneys are the only routes for conservation and elimination of excess water. In conditions of dehydration, the kidneys reabsorb large amounts of water, and excretes excess water not required by the body.
Renal handling of water
The kidneys filter around 180 litres per day, and only 1-2 % of this is excreted as urine. The proximal tubules reabsorb 65% of filtrate regardless of the needs of the body (termed “obligatory reabsorption”); 15% is reabsorbed in the loop of Henle and 20% in the distal nephron (12% of which is under the control of ADH and 8% reabsorbed in the collecting duct).4 The normal rate of urine formation is 1 ml/minute ; a rate of > 2ml/min is diuresis; presenting as polyuria.
Water reabsorption is by osmosis through water channels in the membrane5. These water channels consist of a family of proteins called aquaporin. At least seven different aquaporin isoforms are expressed in the kidney. The proximal tubule has abundant AQP1 on the apical and basolateral membranes and AQP7 on the apical membrane of the late proximal tubule.
The glomerular filtrate is isotonic to plasma (osmolality of 280 + 5 mOsm/kg; taken as 300 for easy calculation). In the total absence of AVP, up to 12% of filtrate is not reabsorbed together with solutes, so the urine becomes diluted. If water is needed and AVP is released, water is reabsorbed. This mechanism is referred to as the “diluting and concentrating power “of the kidneys. Since the urine osmolality ranges from 30 to 1400 mOsm/Kg, the kidneys demonstrate a diluting capacity of 10 times (filtrate diluted from 300 to 30) and concentrating power of 4.5. (filtrate concentrated from 300 to 1400). Loss of concentrating power is therefore the earliest symptoms of renal insufficiency, presenting as nocturia.
The “Osmotic ceiling” is the maximum concentration possible without compromising the kidneys’ role of eliminating osmotically active substances resulting from ingestion of protein. These are around 700 mOsm on a western diet, so at least 500 ml of urine is needed to eliminate these wastes, given an osmotic ceiling of 1400 mOsm/kg. NB- Myanmar people eat less protein and our osmotic load is less; so we are all right with a minimum urine volume of 400 ml/day; “oliguria” is set at 400 ml/day in our setting.
Regulation of ECF volume and tonicity
Three mechanisms defend the ECF volume and tonicity viz. Thirst, Anti-diuretic hormone (ADH; also called arginine vasopressin or AVP) and the renin-angiotensin –aldosterone system (RAS). Thirst results in water being added from external sources. AVP and the RAS add water to the ECF by conservation of filtrate. Dehydration may result from inadequate intake of water or excessive or abnormal losses as hypotonic or isotonic fluids, the result being hypertonic or isotonic dehydration (with reference to plasma osmolality)
The Thirst mechanism
The lateral hypothalamic area, the hypothalamic paraventricular nucleus, and the periaqueductal gray are all regions that receive a strong neural input from the lamina terminalis and have been proposed as regions that may participate in the generation of thirst6.
An increase in plasma osmolality or fall in plasma volume stimulate the thirst centre and release of AVP from the posterior pituitary. Other stimuli include dryness of oro-pharynx (“pharyngeal metering”) . The thirst centre becomes less sensitive in the elderly.
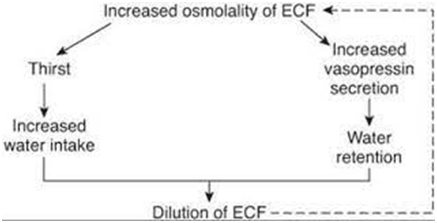
Fig.3– the thirst mechanism and AVP act together to defend the extracellular and osmolality. (Source: WF Ganong. Review of Physiology).
Antidiuretic hormone (ADH) / Arginine vasopressin (AVP)
The late distal tubule and the collecting tubules are made permeable to water by the presence in the circulation of antidiuretic hormone (AVP) released from the posterior pituitary gland .The early distal tubule is not permeable to water and its permeability is not changed by AVP. Stimuli for thirst also stimulate AVP release. Additional stimuli include stress, pain, nicotine, standing up (increase in sympathetic tone), angiotensin II. Surgery stimulates AVP release up to 36 hours post-operation. . AVP release is inhibited by fall in plasma osmolality, plasma volume expansion, alcohol. Inhibition by reduced plasma osmolality is attenuated in the third trimester of pregnancy, allowing the blood volume to expand. Diabetes insipidus is a deficiency of AVP. Large volumes of hypotonic urine are excreted (water diuresis). The polyuria of diabetes mellitus is osmotic diuresis (water is excreted together with the glucose). SIADH is an inappropriate release of AVP i.e. released although the body does not need it, by ectopic sites like tumours , some lung conditions and some drugs.

Fig.4—Stimuli for AVP release and inhibition of release
(Source: WF Ganong Review of Physiology).
The Renin-angiotensin –aldosterone system (RAS).
The RAS regulates both volume and osmolality/ tonicity of the ECF volume. The juxtaglomerular apparatus of the kidneys detects alterations in sodium in the blood and filtrate. It is also stimulated by sympathetic stimulation. A fall in blood volume stimulates the sympathetic system which in turn stimulates the JGA to release renin. Circulating angiotensinogen is cleaved by renin to become angiotensin I (ANG I). Angiotensin converting enzyme (ACE) in the lungs and endothelia convert angiotensin I into the more active angiotensin II (ANG II). ANG II stimulates thirst and release of aldosterone; causes vasoconstriction through the AT2 receptors.(AT1 receptors cause vasodilation) Aldosterone acts on the distal tubules to reabsorb sodium and secrete potassium ( kaliuretic action). Water reabsorption follows sodium reabsorption, to increase the plasma volume.
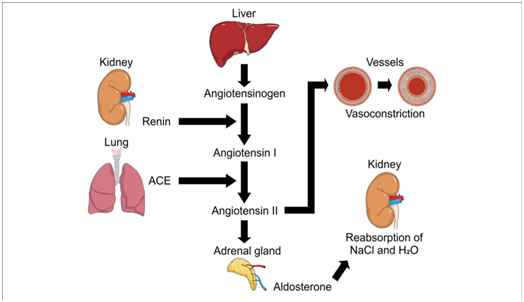
Fig.5-https://www.researchgate.net/figure/Representation-of-Renin-Angiotensin-Aldosterone-System-RAAS-Regulation-mechanism-
Types of dehydration
- Isotonic dehydration is the most common cause. The dehydration is not shared between the compartments and presents with hypovolaemia. Examples of causes are diarrhoea, vomiting, haemorrhage, long-term “nothing by mouth”, gastric suction, fistulae, burns, severe wounds. Isotonic dehydration is confined to the IVF and manifests mainly as reduction in blood pressure and compensatory tachycardia
- Hypertonic dehydration is the next most common type resulting from loss of hypotonic fluid / “pure “water loss. The effects of loss is shared by the ISF and ICF and is not associated with hypovolaemia. Examples: are sweating (sweat is a hypotonic fluid) , hyperventilation, prolonged fevers, diabetes insipidus, end-stage renal failure, tube feeding .ISF dehydration presents as poor skin turgor, (“tenting”) sunken eyes, sunken fontanelle, dry tongue. Cellular dehydration involving brain may present irritability, delirium, hallucinations, loss of consciousness.
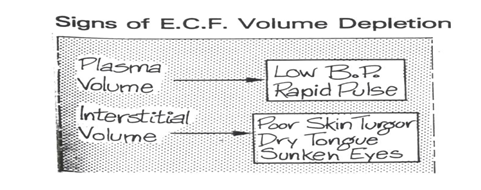
Fig. 6– Signs of ECF depletion (Source: Illustrated Physiology)
Symptoms of dehydration
The first symptoms of dehydration include thirst, darker urine, and decreased urine production. However, it is important to note that, particularly in older adults, dehydration can occur without thirst. This is why it is important to drink more water when ill, or during hotter weather. As the condition progresses to moderate dehydration, symptoms include: dry mouth, lethargy, weakness in muscles, headache and dizziness
Severe dehydration (loss of 10-15 percent of the body’s water) may be characterized by extreme versions of the symptoms above as well as: lack of sweating, sunken eyes, shrivelled and dry skin. Low blood pressure, increased heart rate, fever, delirium, unconsciousness.
(1) In the CVS ( hypovolaemia) :
- Increased pulse rate (rapid, thready pulse) (low BP)
- Postural hypotension
- Flat neck and hand veins in dependent position
- Diminished peripheral pulses
- Weight loss
- In the respiratory: system
- Increased rate of respiration
- Increased depth of respiration
(2) In the gastrointestinal tract
- Decreased motility
- Reduced bowel sounds
- Constipation
(3) Renal
- Thirst
- Highly-coloured urine
- Decreased urine volume
- Increased urine specific gravity
(4) Neuromuscular
- Lethargy
- Restlessness
- Fever
(5) Integumentary
- Skin dry & scaly
- Poor turgor, tenting present
Hypotonic dehydration: may manifest as skeletal muscle weakness and hypertonic dehydration may exhibit hyperactive deep tendon reflexes, increased sensation of thirst and pitting oedema
Symptoms in children
Dehydration in babies can be detected by sunken anterior fontanelle, dry tongue and mouth, irritability, absence of tears when crying, sunken cheeks and/or eyes, and no wet diaper for 3 or more hours.
Evaluation of dehydration
There are many guidelines available online on the evaluation and management of dehydration. Urine colour and weight loss are good indicators for a quick evaluation. Presence of the above-mentioned symptoms are weighed to assess the severity. A thorough history including information on fluid intake and possible extra losses would influence management. Biochemical tests such as plasma and urine osmolality are useful for classifying the type of dehydration and for assessing severity. Glucose and electrolytes shoud be measured to rule out underlying pathology.
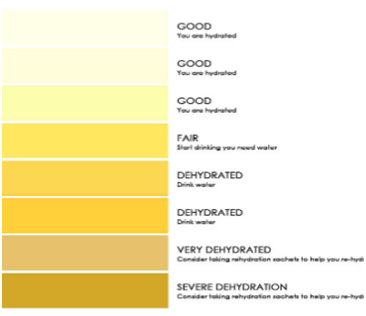
Fig.7 – colour scale urine hydration chart9
Management of dehydration
The problem is loss of water and/or solutes from the body fluid compartments. Obviously, the deficit neds to be corrected. Fluid replacement therapy is a large topic on its own, and is a very specialised field, beyond the scope of this article. Howeer, a few general points are useful. After excluding obvious causes of dehydration from the history (haemorrhage, exposure to extreme temperature, strenuous exercise, debilitating illness, diabetes mellitus, diabetes insipidus, adrenal gland pathology, end-stage renal disease), the severity of dehydration should be evaluated on clinical assessment and biochemical tests and fluid replacement begun. The amount required would depend on the severity (loss of 5% of basal body weight = mild dehydration; 5-10%= moderate dehydration ;>10% = shock). Numerous formulae are available and treatment centres have their own guidelines. An example of key points from guidelines include8:
- Whenever possible, the enteral route should be used
- In most situations, the preferred fluid type is sodium chloride 0.9% (with glucose 5% +/- potassium for maintenance fluid)
- Most sick children will retain water and require less than full maintenance fluids
- Serial weights are the best measure of acute changes in fluid status
It is worthy of note that 0.9% NaCl (“normal saline”) is isotonic to plasma and therefore fluids remain in the IVF. Glucose gets metabolized and the plasma becomes hypotonic, so water moves into the ISF.
References
- Weinberg AD, Minaker KL. 1995. Dehydration. Evaluation and management in older adults. Council on Scientific Affairs, American Medical Association. JAMA. Nov 15; 274(19):1552-6. [PubMed]
- ATobias;BD.Ballard;SS.Mohiuddin2021.Physiology,Water Balancehttps://www.ncbi.nlm.nih.gov
- M Rasouli 2016. “Basic concepts and practical equations on osmolality:, Biochemical approach” https://pubmed.ncbi.nlm.nih.gov/27343561/
- 4. K Brands. 2020. Summary of Renal Water Handling.
https://med.libretexts.org › Anatomy and Physiology - J Feher. 2017. “Water absorption. https://www.sciencedirect.com/ topics/ immunology-and-microbiology/water-absorption
- MJ McKinley & AK Johnson 2004. “The Physiological Regulation of Thirst and Fluid Intake “. https://doi.org/10.1152/nips.01470.2003
- Dehydration: Symptoms, causes ,and treatments –Medical https://www.medicalnewstoday.com › articles
- Good Clinical Practice. Royal Children’s Hospital, Melbourne. https://www.rch.org.au/clinicalguide/guideline_index/Intravenous_Fluids
- AAS Gunawan , D Brandon , VD Puspa b , B Wiweko 2018.
“Development of Urine Hydration System Based on Urine Color and Support Vector Machine” Procedia Computer Science 135. 481–489
Author Information
Hla Yee Yee
MBBS (Rgn); MSc(Mdy); PhD(Lond); FRCP (Edin)(hon)
Honorary Professor, University of Medicine 1, Yangon






