COMISA (Comorbid Insomnia and Sleep Apnea) is a new research area in sleep medicine with emerging evidence of significant effect on CPAP compliance to OSA patients. It had effect on cardiovascular comorbidities reported by many OSA and insomnia-related research trials.
COMISA exacerbates nighttime sleep disturbances, increased day time dysfunctions and further diminishes over all QOL. It is also associated with elevated cardiovascular and mental health risks, including resistant hypertension, hearth failure, stroke, depression and anxiety. Despite its clinical importance, COMISA often remains undiagnosed.
Insomnia and OSA are the two most prevalent sleep disorders and frequently co-exist. Insomnia is a chronic condition persisting for at least three months and characterized by self-reporting difficulties in initiation, maintaining habitual sleep associated with daytime functional impairments.
A recent study in China revealed there was an age association for COMISA particularly in elderly patients with OSA
(Fig 1)
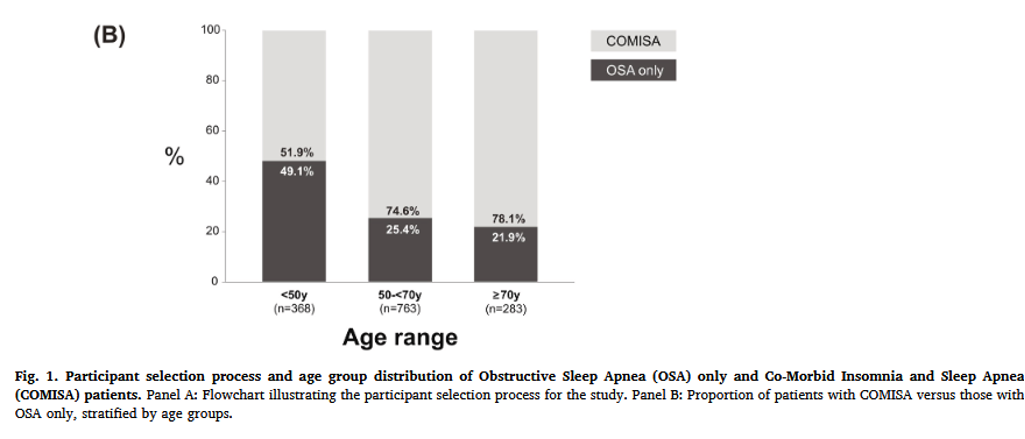
COMISA occurred in approximately 30% to 50 % of insomnia and OSA patient population, prevalence estimate varying by severity threshold, sampling and assessment tools (fig.1).
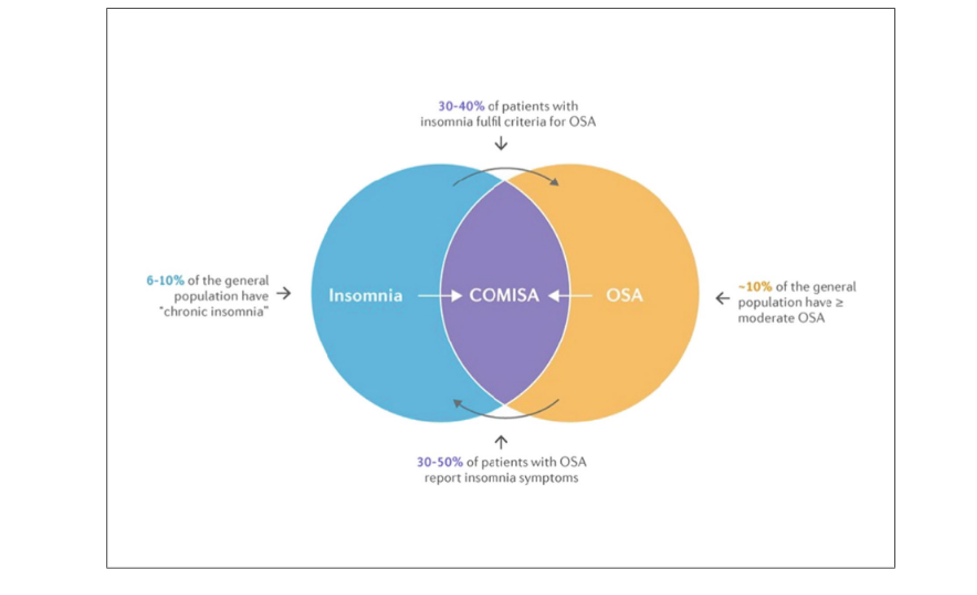
Fig 2. Co-morbid insomnia and sleep apnea (COMISA) is prevalent in 30%-40% of patients with insomnia, and 30%-50% of patients with obstructive sleep apnea (OSA). Figure adapted with permission from Sweetman et al.
Bidirectional relationship between insomnia and OSA.
Interaction between the two conditions may contribute to the development and exacerbation of the other disorders. This may result is greater morbidity and reduced response to treatment of each condition compared to isolated treatment of each.
The hypothesis proposed for this pathophysiology is nocturnal respiratory events, sympathetic drive, cortical arousals and frequent awakening contributed insomnia symptoms. This is supported by cohort studies.
COMISA vs. CPAP compliance in OSA patients
In patients with COMISA, CPAP therapy may exacerbate preexisting insomnia symptoms and may provide less therapeutic benefit if insomnia symptoms persist despite adequate CPAP usage. Patients with COMISA are 30% less likely to accept CPAP compared to those with OSA alone. Recent review identifies an association between adequate treatment of OSA by CPAP with improvement in OSA-related insomnia up to 20% to 50% especially for daytime symptoms.
COMISA vs. Cardiovascular and Cerebrovascular comorbidities
COMISA s associated with a three-fold increased risk of resistant hypertension and heightened cardiovascular morbidities reported by review articles. This is thought to be inflammatory and metabolic dysregulations associated with cardiometabolic sequelae in OSA and insomnia. The last two decades, many studies found that Insomnia with Short Sleep duration (ISSD) phenotype is strongly associated with significant cardiometabolic morbidities, including hypertension, diabetes, cardiovascular diseases and mortality
(Fig 3
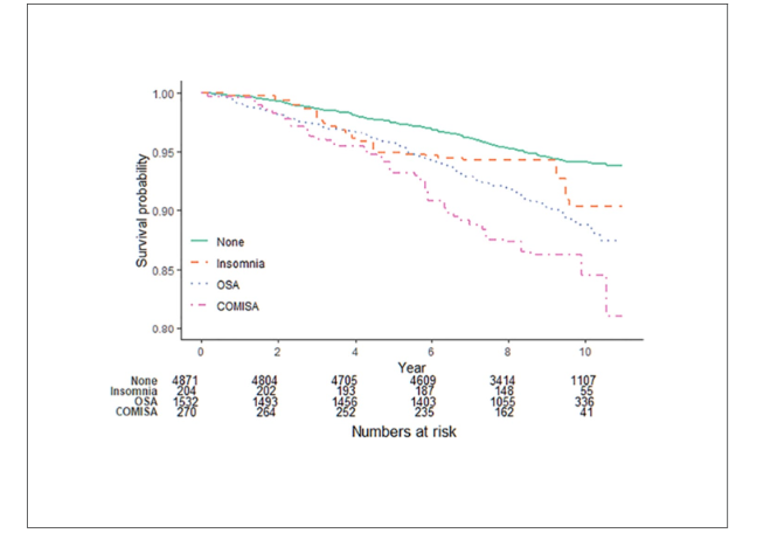
Management of COMISA
Simultaneous management of both conditions is important to prevent burden on comorbidities.
CBTI, Cognitive and Behavioral Therapy for Insomnia are the internationally accepted firstline treatment. Compliance with drug treatment (hypnotics) as directed by AASM insomnia treatment guidelines if CBTI is not feasible.
For OSA, individualized treatment based on international OSA treatment guidelines is required. This will include CPAP, OA (oral Appliance), body weight reduction, corrective surgery, hypoglossal nerve stimulation, myofunctional and other procedure based on current trends.
References;
- Nicolaos et al, (2026) OSA comorbid with insomnia symptoms; journal of clinical sleep medicine 22;11, doi.org.10.0017
- Meina Wu et al; (2024) association between age and comisa; Sleep Medicine 124, 659-661
- The American Academy of Sleep Medicine. International Classification of Sleep Disorders (ICSD-3), Diagnostic and Coding Manual, 3rd ed.; The American Academy of Sleep Medicine: Westchester, IL, USA, 2014.
- Alexander Sweetman et al; (2023)Current sleep medicine reports 9;180-189/doi.org/ 10.1007/s 40675-023-00262-9
Author Information
Zay Ya Aye
MBBS, MMed, Sc. Internal Medicine






