Uncomplicated Falciparum Malaria In Mobile Migrant Populations In Myanmar Bangladesh Border Area: Effectiveness Of Dihydroartemisinin – Piperaquine Therapy
Background
In 2018, an estimated 228 million cases of malaria occurred world-wide, compared with 251 million cases in 2010 and 231 million cases in 20171. Most malaria cases in 2018 were in the World Health Organization (WHO) African Region (213 million or 93%), followed by the WHO South-East Asia Region with 3.4% of the cases and the WHO Eastern Mediterranean Region with 2.1%.1 In 2018, there were an estimated 405,000 deaths from malaria globally, compared with 416,000 estimated deaths in 2017, and 585,000 in 2010. 1
In Myanmar, according to world malaria report, the total number of reported confirmed cases of malaria was nearly 80,000 and the number of reported death cases was thirty in 2017(2). Confirmed falciparum malaria cases per 1,000 population was 50 – 100 in Rakhine and Chin State and the figure was higher in some areas 2.
On the other hand, artemisinin resistance has been confirmed in the Greater Mekong Sub region (GMS), emerging in the same location as resistance to earlier anti-malarial drugs. 3 Thus, the strategy for malaria elimination in the Greater Mekong Sub region (2015–2030) has been launched by WHO since 2015.4 The drug resistance has hastened the commitment of GMS countries to eliminate malaria by 2030. Moreover, population mobility is a key priority for addressing drug resistance, but a range of challenges has inhibited the capacity for countries to effectively engage migrant and mobile populations (MMPs)5. Regarding population mobility and malaria, WHO reviewed international, regional and national policies and legal frameworks which enhance MMPs access to health and malaria services in the Greater Mekong Sub region- Cambodia, Lao People’s Democratic Republic, Myanmar, Thailand and Viet Nam.6 In 2016, World Health Organization advised several approaches for MMPs in the context of malaria multi-drug resistance and malaria elimination in the GMS.7 In border malaria meeting report by evidence review group, there were multiple factors including political unrest, difference of social and economic development, weak surveillance and response systems, insufficient access to health service, and differences in national malaria policies, treatment-seeking behaviours and other factors can contribute to malaria transmission in border areas.8,9
Generally, the border areas tend to have the least-developed health systems of the nation.10 As the country seeks malaria elimination, the last remaining infection foci often occur along the international borders, we should address border malaria early in our elimination efforts. 10 The studies on border malaria had mentioned several difficulties in treating MMPs. 11,12 The spread of artemisinin resistant malaria was reported by some trials 14 and it was also found in Myanmar 15. There were several challenges in malaria elimination16 and the border malaria cases were in state of increasing trend.17The study in Cambodia also highlighted the magnitude of MMPs.18
In Bangladesh, the major investment was done for malaria elimination.19 The MMPs migration 20, 21 and the prevalence of malaria 22 were also described in their studies. Nepal, borders with Bangladesh and India, designed on control of MMPs. 23 BBC news also mentioned that India was threatened by the spread of artemisinin resistant malaria from Myanmar 24 as the resistant cases were reported in Myanmar. 27
Regarding the treatment, the fixed dose antimalarial combination of dihydroartemisinin-piperaquine (DP) is one of the artemisinin-based combination therapy (ACT) recommended in both WHO and national guideline for the treatment of uncomplicated falciparum malaria 3, 13. Not only the studies on border malaria 26 but also the meta-analysis of the studies done in GMS and Africa 25 showed that it was safe and effective 28-33. The effectiveness of DP in Myanmar China border revealed that it was good too 26. However, there were limited reports on MMPs in Myanmar Bangladesh border area. Thus, this study aimed to detect the effectiveness of DP in MMPs in Myanmar Bangladesh border area.
Methods
Study site and populations
It was done in the Warnetyon village, 5 miles away from Myanmar Bangladesh border. The village is under the Butheetaung township area, Rakhine State. It is 20 miles away from Butheetaung Township. The Warnetyon village borders between Bangladesh and Chin state/Rakhine State (Myanmar). It is situated in hilly region which are continuous with mountains from Rakhine State and Chin State. It is also close to the Chittagong Hill Tracts areaof Bangladesh which is reported as malaria hyper-endemic area with a prevalence of 11% or even higher 22. The study period was March 2018 to October 2019.
The Warnetyon village has approximately 100 houses with 200 villagers. The nationalities are mainly Chin (Myo and Dinet) and the minority is Myanmar (migrant population- 5%). It takes several days if we walk from the Buthitaung township to reach the Warnetyon village although it is only 20 miles away. Although the transport with motor vehicles takes 5 hours from Butheetaung township to the Warnetyon village, the people have to walk to avoid disturbance from insurgents. The duration of travelling time varies – it takes two days walk in the dry season and five days walk in the rainy season. The Warnetyon village is also hot as it is close to the Palawa township of Chin State where there were several confirmed cases of malaria in 2016-2017. Though the Palawa township is situated 50 miles east of the Warnetyon village, there is no road to the Palawa township. Being very hard to reach area, most of the mobile populations were soldiers and the road construction workers. The natives rarely travel to the Butheetaung Township because of logistics – transport difficulties and security reasons. The mobile population was moving owing to their duties. The migrant population was doing business by opening small groceries shop in the Warnetyon village. The imported foods were very expensive. The cost of one packet of coffee mix was 500 kyats in the Warnetyon village compared to 100 kyats in the Butheetaung township. Most of the people had to depend on locally available products like stone water melon and preserved fish.
All cases with fever and chills, suspicious of malaria, first seen at the mobile clinic were referred to the unit clinic. The unit clinic was based at the center point of the Warnetyon village which can accommodate 20 beds for in-patients care. The unit clinic team is composed of 8 members: one physician, three nursing brothers, 3 nursing assistants and one clerk. The unit clinic team was connected with five mobile clinics. Each mobile clinic consisted of 5 members: one doctor, one nursing officer-brother, 2 nursing assistants and one clerk. The members of the mobile clinic were moving along with mobile people around the Warnetyon village. If the patients seen in the mobile clinic required in-patient treatment, they were brought to the unit clinic based in the Warnetyon village. They were referred again to the clinic based in the Butheetaung Township where they got better care. If necessary, they were sent to the Sittwe District hospital where they could get ventilator support for patients. The post mortem examination was performed in the Sittwe District hospital. Some cases were referred to Mingaladon General Hospital (1000 Bedded) for renal replacement therapy. All the team members did communicate with each other through mobile phone. They were supervised by clinical research unit based in Mingaladon General Hospital (1000 Bedded).
Study design and data collection
It was a unit clinic based descriptive study done in the Warnetyon village .Those patients having fever (axillary temperature ≥ 37.5 °C) were screened at unit clinic. The patients having history suggestive of flu like symptoms were excluded. After taking history and physical examination, blood was taken from the finger tip for rapid test-ICT malaria. Those with positive test for falciparum were included. Those having features of complicated malaria like confusion, black water fever, hypotension were excluded. Demographic (ethnicity, age, gender, occupation, education, travel history) and clinical (fever, fever history, symptoms, malaria history, previous treatment) data were obtained using a structured questionnaire. Written informed consent was obtained from all participants, prior to enrollment into the study. Then, oral Artequine 3 tablet once a day for 3 days was prescribed under supervision in the unit/mobile clinic. It was produced from Tatmadaw Pharmaceutical Factory. Each tablet contains 50 mg dihydroartemisinin and 350 mg piperaquine. Antipyretics (Paracetamol 500 mg p. r. n) and anti-emetics (Metoclopromide 5 mg prn) were given if necessary. Dehydration was corrected accordingly. Temperature was recorded 12 hourly till the patient was afebrile for 48 hours. Then it was recorded daily till 21 days.
If the patient developed fever again, possible source of infection (e.g.pneumonia) was looked for again. If no apparent cause was found, rapid test for malaria was repeated again. If vivax malaria was positive, chloroquine three day course was given. If no apparent cause was detected and vivax was negative in rapid test, they were diagnosed as possible clinical relapse and treated with Co-artem (Artemether-Lumefantrine) according to body weight. The patient was discharged from unit/mobile clinic if he was apyrexial for two weeks and follow up was done weekly till 42 days via mobile/unit clinic physician.
The data entry was done by physicians. Simple statistical analysis was done after data cleaning. The working definitions used for this study were slightly different from WHO definition as the study was performed in the Warnetyon village-very remote area.
Results
Table [1] Malaria Screening Statistic in the Warnetyon village

Table [1] Malaria Screening Statistic in the Warnetyon village
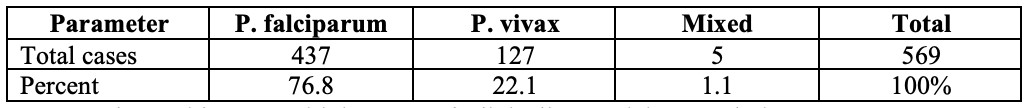

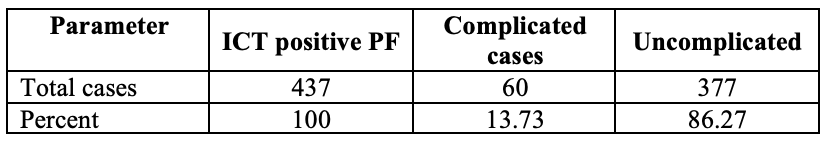
The rapid test positivity rate of clinically suspicious malaria cases was 72.48% and falciparum malaria account 76.8%. Among falciparum malaria cases, those having features of complicated form was 60 (13.73%).
Table [3] Frequency distribution of ICT positive P. falciparum cases by severity ( n=437)
There were no serious side effects.
Discussion
The prevalence of malaria was generally falling except in some areas 1, 2 and the mortality rate was not zero2. The problem of artemisinin resistance in the Greater Mekong Sub region (GMS) and its spread was a worrisome situation 3. One of the important determinants of spread of drug resistant malaria was population mobility 8,9. It was found to be key issue in the border areas especially very hard to reach one. Usually, they had the least-developed health systems of the nation 10. As we aimed for malaria elimination in 2030, dealing with MMPs and spread of drug resistant malaria were paramount important. 7-9
In this study, the percentage of positive rapid test among clinically suspected malaria cases was 72.48% (569/785). Because of difficulties in electricity and the other logistic issue, the microscopic confirmation was not able to perform. The number of clinically suspicious cases was very high among mobile population as they were non-immune. However, the percentage of rapid test positive cases were comparable with that of Myanmar malaria profile where the confirmed falciparum malaria cases per 1,000 populations was 50 – 100 in Rakhine and Chin State.2
As the study area was only 5 miles away from Bangladesh border, the malaria situation in Bangladesh side was interesting. According to the epidemiological overview of malaria in Bangladesh in 2013, it was one of the malaria endemic countries and over 34% of population was at risk to malaria 22. The Chittagong Hill Tracts area was said to be hyper-endemic with a prevalence of 11% or even higher. As it was close to mountains from Rakhine State and Chin State on our side, it was also alarming for us. The health sectorin Bangladesh was worried about hidden migration and services for mapping was reinforced 20, 21. Thus, they did major investment in malaria elimination19. Regarding treatment, like Myanmar, the Artemether – Lumefantrine combination therapy was the main artemisinin combination therapy used for the treatment of uncomplicated falciparum malaria 22. The bad point was that if the parasite became resistant to current treatment, both countries had to change treatment policy.
With reference to the dominant malaria species, the proportion of falciparum malaria was 76.8% (437/569) and that of vivax was 22.1% (127/569) in this study. Again it was comparable with national figure – 68% and 31% respectively 2. Nevertheless, the study done in Myanmar -China border revealed that the proportion of vivax malaria was high 26. It was contrary to our finding. It could be due to different study site- eastern part and western part of Myanmar. In Bangladesh, the number of cases with falciparum malaria was greater than that of vivax malaria 22. Thus, falciparum malaria was the main problem in national control programme of Bangladesh. It showed that border malaria had several similarities as they were dealing with same temperature, climate changes, humidity and ecology 8,9.
In present study, those having features of complicated falciparum malaria was 13.73% (60/437) and all were mobile population. They suffered fever with severe features 2–3 months after arrival to the Warnetyon village. None of severe cases were seen in native people. Therefore the possible reason for protection from complicated falciparum malaria would be related with immunity. Moreover, majority of them were in real mobile situation is not settling in base. The reason was that they could not use preventive measures like bed net or mosquito coil. In fact, they rarely used repellant. It would be the main reason for acquiring malaria.
About the cured rate, it was scientifically defined by WHO as adequate clinical and parasitological response rate in day 42. However, we had to use possibly cured rate for logistic reasons. It was defined as “those patients who do not have recurrence of fever till 42 days with improvement of other symptoms like general wellbeing, appetite and normal urine output.” Early clinical failure was defined as those having recrudescence of fever within two weeks plus no apparent cause for fever in lung, skin and urine plus rapid test negative for vivax malaria. Late clinical failure was defined as those having recrudescence of fever after two weeks plus no apparent cause for fever in lung, skin and urine plus rapid test negative for vivax malaria. In this study, ten cases had recurrence of fever on day 10 and they received artemether-lumefantrine therapy. There was no late clinical failure case. The possible cure rate in this study was nearly 95%.
The artemisinin combination therapy – DP was one of the recommended treatments for uncomplicated falciparum malaria for almost 10 years 13. There were many therapeutic efficacy trials on dihydroartemisinin-piperaquine (DP) 26-33. In the prospective multi-centre individual patient data analysis done over studies conducted in Africa and South East Asia, DP was superior to the comparator drugs (mefloquine-artesunatein Thailand, Myanmar, Laos and Cambodia; artemether-lumefantrine in Uganda; and amodiaquine+sulfadoxine-pyrimethamine and artesunate+amodiaquine in Rwanda) in protecting against both P.falciparum recurrence and recrudescence 25. There were less adverse events with DP 28-33. The bad point was that the proportion of patients developing gametocytaemia and the subsequent gametocyte carriage rates were higher with DP than its comparators 25. In this study, we could not perform microscopy and thus could not detect it.
Another study done in Myanmar- China border area showed that DP was effective too 26. Also in our own studies done in various areas of Myanmar revealed that DP was 95-100% effective (42 days PCR corrected ACPR) and very safe. 28-33
With regard to border malaria, it was not an easy issue for all malaria endemic countries.There were several approaches suggested for control of border malaria.7-9 Every country admitted that they were afraid of spreading artemisinin resistant malaria 22- 26. They were blaming their neighbors. It was clear that the report from India study on border malaria, India was worried about imported cases from Bangladesh and Myanmar 24. Also, that of Bangladesh explained that difficulties in tracing MMPs in own country 20, 21. The study done in China-Myanmar pointed out that the malaria cases were draining from Myanmar 26. Also, Thai–Myanmar border study blamed imported cases from Myanmar 11,12.
In fact, MMPs was very difficult to treat and several countries explained their experiences like Nepal 23 and Cambodia 18. In one report, the transmission dynamic and vulnerability of MMPs to multi-drug resistance malaria had been pointed out and the importance of the surveillance had been mentioned in Thailand-Myanmar and Thailand-Cambodia Borders 11. In the study done in MMPs of Myanmar mentioned malaria case detection among mobile populations and migrant workers in Myanmar- Bago Division, Rakhine State and Thai border 12.
In this study, there were only very minor side effects like giddiness. There was no cardiovascular adverse event. It was the same finding in previous studies 28-33.
Conclusion
Therefore, the possible cure rate was nearly 95% in this study. It can be concluded that dihydroartemisinine–piperaquine therapy (DP) was still effective in treatment of uncomplicated falciparum malaria in mobile migrant populations (MMPs) in Myanmar Bangladesh border area – the Warnetyon village. Itwas a safe and well tolerated, and highly effective treatment of P.falciparum malaria in MMPs in Myanmar Bangladesh border area.
Weakness of the study
As the Warnetyon village was very remote area we could not do microscopy. We did not give primaquine asgametocidal drug because their G6PD status was not known.
Acknowledgement
We would like to thank all patients, physicians, nursing brothers, nursing assistants and administrators for their active participation in this study.
References
- World Health Organization (WHO), World malaria report 2019 December.
- World Health Organization (WHO), Country profile Myanmar 2018
- World Health Organization (WHO), Artemisinin and artemisinin-based combination therapy resistance. Status report. Geneva: World Health Organization; 2016. http://www.who. int/malaria/publications/atoz/update-artemisinin-resistance-april2016/ en/. Accessed 28 Jun 2016.
- World Health Organization (WHO), Strategy for malaria elimination in the Greater Mekong Subregion (2015–2030). Geneva: World Health Organization; 2015.
- World Health Organization (WHO), Regional Office for South-East Asia. Approaches for Mobile and Migrant Populations in the Context of Malaria Multi-Drug Resistance and Malaria Elimination in the Greater Mekong Subregion. Geneva: WHO; 2016. http://apps.who. int/iris/handle/10665/204351. Accessed April 16, 2018
- World Health Organization (WHO), Population mobility and malaria. New Delhi: World Health Organization, Regional Office for South-East Asia; 2017. Licence: CC BY-NC-SA 3.0 IGO
- World Health Organization (WHO), Regional Office for South-East Asia. Approaches for Mobile and Migrant Populations in the Context of Malaria Multi-Drug Resistance and Malaria Elimination in the Greater Mekong Subregion. Geneva: WHO; 2016. http://apps.who.int/iris/handle/10665/204351. Accessed April 16, 2018.
- World Health Organization (WHO), Geneva, Switzerland; Evidence review group on border malaria Meeting report, 10–11 May 2018
- World Health Organization (WHO). Mobile and migrant populations and malaria information systems; 2015
- Inkochasan M, Gopinath D, Vicario E, Lee A, Duigan P. Access to health care for migrants in the Greater Mekong subregion: policies and legal frameworks and their impact on malaria control in the context of malaria elimination. WHO South-East Asia J Public Health. 2019;8(1):26–34. doi:10.4103/2224–3151.255346
- A Bhumiratana, A Intarapuk, P Sorosjinda-Nunthawarasilp, P Maneekan, and S Koyadun, “Border Malaria Associated with Multidrug Resistance on Thailand-Myanmar and Thailand-Cambodia Borders: Transmission Dynamic, Vulnerability, and Surveillance,” BioMed Research International, vol. 2013, Article ID 363417, 13 pages, 2013. https://doi.org/10.1155/2013/363417.
- Kheang T, Lin M A, Lwin S, Naing Y H, Yarzar P, Kak N, et al. Malaria case detection among mobile populations and migrant workers in Myanmar: comparison of 3 service delivery approaches. Glob Health SciPract. 2018;6(2):381-386. https://doi.org/10.9745/GHSP-D-17-00318
- Myanmar Ministry of Health.National malaria treatment guidelines. Nay Pyi Taw: Department of Health, Ministry of Health; 2009.
- Ashley EA, Dhorda M, Fairhurst RM, Amaratunga C, Lim P, Suon S, et al.Spread of artemisinin resistance in Plasmodium falciparum malaria. N Engl J Med. 2014;371:411–23.
- Kyaw MP, Nyunt MH, Chit K, Aye MM, Aye KH, Aye MM, et al. Reduced susceptibilityofPlasmodium falciparum to artesunate in southern Myanmar. PLoS ONE. 2013;8:e57689.
- L Cui, Y Cao, J Kaewkungwal, A Khamsiriwatchara, S Lawpoolsri, T N Soe, M P Kyaw& J Sattabongkot (July 18th 2018). Malaria Elimination in the Greater Mekong Subregion: Challenges and Prospects, Towards Malaria Elimination – A Leap Forward
- G Jinting , M Pallavi , Z Jiaqi , X Shiling , L Cuiying ,Z Yan, W Qinghui , M P K, C Yaming , Y Zhaoqing& C Liwang. Increasing trends of malaria in a border area of the Greater Mekong Subregion Malar J (2019) 18:309
- Guyant P, Canavati SE, Chea N, Ly P, Whittaker MA, Roca-Feltrer A, Yeung S.Malaria and the mobile and migrant population in Cambodia: a population movement framework to inform strategies for malaria control and elimination. Malar J. 2015 Jun 20;14:252. doi: 10.1186/s12936-015-0773-5.
- Fox, K., Baral, R., Khan, W., Ching, S.P., Celhay, O., Mercado C., Kyaw, S.S., Silal, S., White, L., Maude, R., Shretta, R. (2017). An investment case for eliminating malaria in Bangladesh. San Francisco: The Global Health Group, University of California, San Francisco
- C Hsiao-Han , W Amy , S Ipsita ,J G Christopher, M Ayesha , U Didar, Z S Ibna , H Md Amir, F M Abul , G Aniruddha ,S A Abu ,R M Ridwanur,IAkramul , K M Jahirul ,R M Kamar ,S A K Mohammad ,J S Tahmina, M MAktaruzzaman, D Eleanor ,A S Gonc, K Mihir ,D Mehul ,V Ranitha,MOlivo ,E-M Kenth ,K Dominic , M J Richard ,B Caroline . Mapping imported malaria in Bangladesh using parasite genetic and human mobility data. eLife 2019;8:e43481
- Xin Lu, David J. Wrathall, Pål Roe Sundsøy, Md. Nadiruzzaman, Erik Wetter, Asif Iqbal, Taimur Qureshi, Andrew Tatem, Geoffrey Canright, KenthEngø-Monsen, Linus Bengtsson. Unveiling hidden migration and mobility patterns in climate stressed regions: A longitudinal study of six million anonymous mobile phone users in Bangladesh. Global Environmental Change 38 (2016) 1–7
- Islam N, B Stefanos ,K N Georgios, An epidemiological overview of malaria in Bangladesh . Travel Med Infect Dis. 2013;11(1):29-36 23. L S Jennifer, G Prakash ,R RKomal ,M Alysse ,H Sara ,A P Ricardo , T D Garib ,A Nabaraj , S T Upendra , B R Megha ,L K Bibek ,O J Jerry & B Adam . Designing malaria surveillance strategies for mobile and migrant populations in Nepal: a mixed‑methods study. Malar J (2019) 18:158
- J Gallagher. Malaria on Myanmar-India border is ‘huge threat’; BBC News ; 20 February 2015
- Zwang J, Ashley EA, Karema C, D’Alessandro U, Smithuis F, et al. (2009) Safety and Efficacy of Dihydroartemisinin-Piperaquine in Falciparum Malaria: A Prospective Multi-Centre Individual Patient Data Analysis. PLoS ONE 4(7): e6358. doi:10.1371/journal.pone.0006358
- Y Wang, Z Yang, L Yuan & et al. Clinical Efficacy of Dihydroartemisinin–Piperaquine for the Treatment of Uncomplicated Plasmodium falciparum Malaria at the China–Myanmar Border ; Am. J. Trop. Med. Hyg., 93(3), 2015, pp. 577–583
- M K Myint, C Rasmussen, A Thi, D Bustos, P Ringwald& K Lin. Therapeutic efficacy and artemisinin resistance in northern Myanmar: evidence from in vivo and molecular marker studies. Malar J (2017) 16:143 DOI 10.1186/s12936-017-1775-2
- K P Pyar,W W Myint, M P Kyaw, M Nyunt& M Than. Efficacy and safety of Artemisinin- Piperaquine (Artekin) compared to Artesunate- Mefloquine(Arequin ) in uncomplicated falciparum malaria in adults Myanamr Health Sciences Research Journal 2007.
- K P Pyar, S A Hla, T M Hlaing, K Z Oo, M Z Myint& M Than. Efficacy and safety of Piperamisinin (Dihydroartemisinin- Piperaquine) in uncomplicated falciparum malaria in adults. ). P43, Myanmar Health Science Research Congress, January, 2011.
- W WMyint, K P Pyar& M Than A study of clinical efficacy and safety of Artepip (Dihydroartemisinin and Piperaquine) in uncomplicated falciparum malaria in adults (2006) ) 14h Myanmar Medical Specialities Conference ,MMA. January 2008
- K P Pyar, S A Hla , Z N H Ag & T M HlaingEfficacy and safety of dihydroartemisinin-piperaquine for the treatment of uncomplicated Plasmodium falciparum malaria in Kyaing Tone township (Eastern Shan State) (2011) 40h Myanmar Health Research Congress ,P32,January 2012
- K P Pyar, S A Hla, S W Hlaing& C A Ag. Efficacy and safety of Dihydroartemisinin-Piperaquinefor the treatment of uncomplicated Plasmodium falciparum malaria in Homalin (Sagaing Division) (2014) 44th Myanmar Health Research Congress ,P24,January 2016
- K P Pyar, S A Hla ,S W Hlaing, C A Aung , N L Mg & L M Mg. Clinical study on efficacy and safety of Dihydroartemisinine – Piperaquine in uncomplicated falciparum malaria in adults in Loikaw2017. ASEAN Military Medical Conference 2019
Author name, degree and designation
- KhinPhyuPyar
M.B.,B.S (Rgn), M.Med.Sc (Internal Medicine), M.R.C.P (UK), M.R.C.P.I (Ireland), F.R.C.P (Glasgow), F.R.C.P.I (Ireland), D.T.M&H (London), Dip.Med.Edu
Professor & Head of Medicine / Professor& Head of Nephrology / Senior Consultant Physician / Head of Clinical Wing/ Head of Clinical Research Unit
Defence Services Medical Academy / No(1) Defence Services General Hospital - Lay MaungMaung
M.B.,B.S (D.S.M.A), M.Med.Sc (Internal Medicine), M.R.C.P (UK ), Dip.Med.Edu
Assistant Lecturer
Defence Services Medical Academy - Tin HtayOo
M.B.,B.S (D.S.M.A), M.Med.Sc (Mental Health)
Medical OfficerNo(8) Medical Battalion, Sittwe - Than Htike
M.B.,B.S (D.S.M.A), M.Med.Sc (Internal Medicine)
Medical Officer
No(8) Medical Battalion, Sittwe - Aung KoKo
M.B.,B.S (D.S.M.A), M.Med.Sc (Paediatrics)
Medical Officer
No(8) Medical Battalion, Sittwe - Aung Myint Thu
M.B.,B.S (D.S.M.A), M.Med.Sc (Internal Medicine)
Medical Officer
No(8) Medical Battalion, Sittwe - Win KyawSoe
M.B.,B.S (D.S.M.A), M.Med.Sc (Internal Medicine), M.R.C.P (UK )
Medical Officer
No(8) Medical Battalion, Sittwe - Nyan Linn Maung
M.B.,B.S (D.S.M.A), M.Med.Sc (Internal Medicine), M.R.C.P (UK ), F.R.C.P (Glasgow)
Consultant Physician
Clinical Research Unit
No(1) Defence Services General Hospital - Zar Ni Htet Aung
M.B.,B.S (D.S.M.A), M.Med.Sc (Internal Medicine)
Consultant Physician
Clinical Research Unit
No(1) Defence Services General Hospital - Sai AikHla
M.B.,B.S (Mdy), M.Med.Sc (Internal Medicine), Dip. Med.Edu
Consultant Physician
Clinical Research Unit
No(1) Defence Services General Hospital

